What’s the difference in rheumatoid arthritis (RA) and "regular" arthritis?
Rheumatoid arthritis is a chronic, systemic, inflammatory arthritis. Someone with RA will usually have what is known as inflammatory joint pain. Inflammatory joint pain presents as swelling and prolonged stiffness of the joints, especially first thing in the morning. The stiffness typically lasts close to one hour or longer and improves with activity.
The small joints of the hands and feet, especially the more proximal (those closest to the wrist and ankle) joints, are commonly involved. Symptoms will usually progress to involve joints bilaterally (on both sides of the body). RA typically does not affect the lower back or the distal joints of the fingers. Rheumatoid arthritis can also affect other organs of the body, including the lungs.
Osteoarthritis, or "regular" arthritis, is a progressive degenerative disease that is characterized by dull joint pain that worsens with activity. Osteoarthritis often affects the hands, low back, and weight-bearing joints of the legs. The joints of the hands commonly affected by osteoarthritis include the base of the thumb and the distal (those farthest away from the wrist) joints of the fingers. Patients may have some morning stiffness in various joints that usually lasts less than 30 minutes.
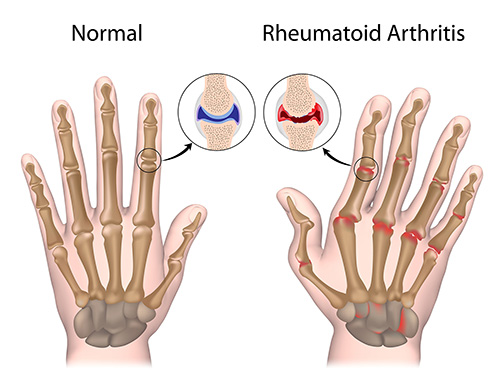
What are the early symptoms of RA?
Most patients present with a slow, gradual onset of pain, swelling, and stiffness of various joints. The small joints are usually symptomatic first, including:
- Metacarpophalangeal (MCP) joints, or knuckles, where the finger bones meet the hand bones
- Proximal interphalangeal (PIP) joints, which are the first joints of the fingers
- Wrists
- Metatarsophalangeal (MTP) joints, which are the joints between the foot and the toes.
Larger joints generally become symptomatic after small joints; however, this is not always the case. Patients may start out with only a few joints involved but then progress to involve multiple joints in a symmetric distribution. The number of joints affected typically increase over weeks to months.
How is RA treated?
The goal in treating RA is to achieve low disease activity – or even remission – and prevent joint damage. We have numerous medications available to achieve this goal. We typically start the patient on a conventional DMARD, which stands for disease modifying anti-rheumatic drug.
Some of the newer medications advertised on television fall into a category of biologic DMARDs or targeted synthetic DMARDs, which work on a certain component of the immune system to control inflammation. These medications can be added if the patient’s RA is not controlled with conventional DMARD therapy.
How can RA affect other parts of your body besides her joints?
RA, especially in those with positive rheumatoid factor or CCP antibodies, can affect other organs in addition to the joints. RA can cause issues with the eyes, lungs, heart, and skin.
Patients can develop inflammation of the eyes, especially of the sclera, which can have serious consequences if left untreated.
The lungs can become affected in multiple ways, including inflammation and fluid around the lining of the lungs, nodules in the lungs, and even interstitial lung disease.
Pericarditis is the most common cardiac manifestation of rheumatoid arthritis. Patients with rheumatoid arthritis are at an increased risk for coronary artery disease compared to those without rheumatoid arthritis.
What’s the prognosis for those with rheumatoid arthritis?
Before the use of modern therapeutic approaches, patients had a worse prognosis with significant disability due to joint damage. Now, with the development of multiple medications to successfully treat RA, we have seen a decline in mortality rates as well as a reduction in disability.
The prognosis of RA is multifactorial. Those with long disease duration prior to treatment have an increased risk for joint damage. Those with a positive rheumatoid factor and CCP antibody are also at an increased risk for a more severe disease course. It is very important for patients to get treated early to try to prevent permanent joint damage. The best results are seen when rheumatoid arthritis patients are started on therapy within 3 to 6 months of the onset of joint symptoms.
What can someone do to help manage their condition?
The most important thing a patient with RA can do is maintain routine follow-up with their medical providers and be compliant with their medications. Since medication therapy is adjusted based on disease activity, it is important to have routine follow-up care to assess for joint swelling and tenderness on exam.
Smoking cessation is another important thing to do for anyone with rheumatoid arthritis. Smoking is an environmental risk factor for RA and is the only modifiable risk factor to reduce the risk of RA.
What else would you like people to know about RA?
We have come a long way with the treatment of RA. Before the development of the available drugs, the prognosis of RA was not great. We now have many options of medications to use to control the disease process and prevent the joint deformities that can occur with RA. The key is to recognize it early and start treatment early before the patient develops any significant disability.

Sallie Giblin, MD, Lexington Rheumatology
Lexington Rheumatology is a Lexington Medical Center physician practice dedicated to treating joint and soft tissue diseases.





Leave a comment